29 / March / 2020 : 00-26
I was initially skeptical of COVID-19. Today, it frightens me.

I am an internal medicine resident working at a nest blanket hospital in New York City. Ten days ago, we had zero patients with COVID in our hospital. Today, we have hundreds. Ten days ago, we were well rested with a supercharged attitude, ready to tackle the virus head on. Today, we are overburdened, exhausted, sick, and disappointed. Our supplies have dwindled, our census of critical patients has skyrocketed, and we are running out of healthcare providers due to the lack of adequate protective equipment. We are fighting a losing battle with no end in sight and need help – now.
Officially, we have 13 resident physicians at this hospital who fallen sick to the virus. Unofficially, it is likely much, much higher. As I walk through the halls, I see attendings and residents hiding their coughs, clearing their throats under their breath, or sniffling as they turn away. Why do we continue to work? Because if we don’t, who will? We are physically sick, but no one can replace us. We hide our emotions and our coughs from our fellow colleagues and try to comfort each other, but we don’t know how. All our energy is focused on our patients.
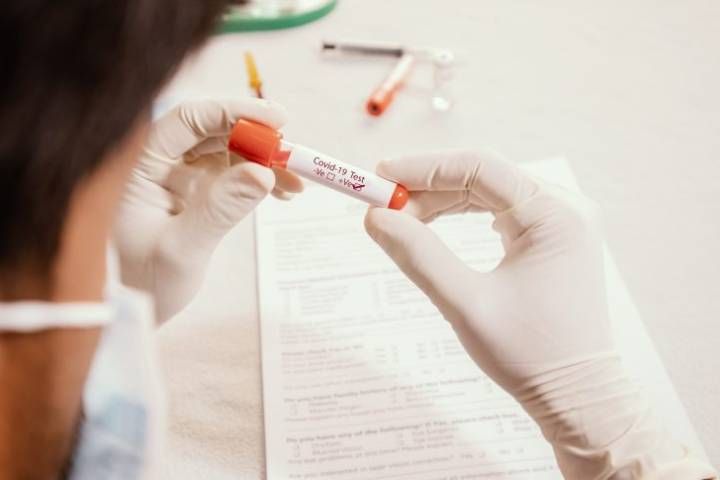
A few days ago, I was called into a code blue. Normal protocol requires that we bag mask the patient, but new COVID protocols state that we should not to avoid aerosolization of viral particles. As I watched him decompensate, I asked myself, “Do I protect my life, or risk his, a 41-year-old with a family and long life ahead of him?” We took an oath when we graduated medical school, and that is why we are here every day. That is why I decided to risk my life to bag mask him.
We have shut down multiple units in our hospital and dedicated them to the care of COVID patients. We call these areas the “COVID Caves.” Each day while working in the ICU, we get an average of 12 new consults for COVID patients. To find them, I walk down a dark hallway, past an endless row of stretchers until I find my new patient. When I reach the gurney propped up against the musty gray wall, I put on my mask, the same mask I have been using for days, and my suboptimal goggles, which I sanitize after each patient encounter. The patient has the “COVID appearance of doom.” We know he will require intubation soon. But we must then decide – how can we allocate our dwindling resources most ethically and effectively? We have already run out of ventilators in this hospital. We cannot provide everyone with the care they deserve. Multiple times per day, we are now faced with the nightmarish and chilling decision of choosing between intubating a 40-year-old patient and an 80-year-old patient. We took an oath to do no harm and act in the best interest of our patients. This country’s lack of preparedness, though, has made it so we cannot act in their best interests. We are here, making life and death decisions, because our markets and governments are systematically broken.
These are not tales from another country. These are truths from New York, your New York. And, soon, this will be the reality in your own town if major changes are not made across the country.
What do we need? We need supplies for patients – ventilators, beds, and medications. We need protection for medical providers – appropriate masks, goggles, and gowns. We need more providers so that those who are sick can stay home to heal and prevent the spread of infection. We need you to take hygiene and distancing protocols seriously. We are begging for help.
Viewed
5999times
Recommended
16 / September / 2020
Kim Kardashian West will freeze her Instagram to protest Facebook
Kim Kardashian West, who has one of the biggest Instagram followings in the world, said Tuesday that she would be joining other high-profile users in a protest against Instagram's parent company...
22 / May / 2026
"The Bank is no Longer Just a Lender, but a Strategic Business Partner": Onik Chichyan
Today, the banking system has entered a phase where digital solutions and speed are no longer the only priorities for customers; strategic partnership with their bank has become paramount. Onik...
23 / October / 2020
The U.S. Mission in Turkey has received credible reports of potential terrorist attacks and...
Security Alert: U.S. Mission in Turkey
Ankara, TurkeyOctober 23, 2020
Event: The U.S. Mission in Turkey has received credible reports of potential terrorist attacks and kidnappings against U.S....
18 / March / 2020
Love in the time of coronavirus: How to live together under lockdown
A freezer packed with food. Tins bulging from kitchen cupboards. Wine, whisky and beer stashed away for when only that dull haze will do.
But after the frenetic days of preparing for lockdown, what...
18 / March / 2020
Love in the time of coronavirus: How to live together under lockdown
A freezer packed with food. Tins bulging from kitchen cupboards. Wine, whisky and beer stashed away for when only that dull haze will do.
But after the frenetic days of preparing for lockdown, what...
18 / March / 2020
Love in the time of coronavirus: How to live together under lockdown
A freezer packed with food. Tins bulging from kitchen cupboards. Wine, whisky and beer stashed away for when only that dull haze will do.
But after the frenetic days of preparing for lockdown, what...
16 / March / 2020
How the new coronavirus could change our behaviour
We’ve all experienced it during these times of the coronavirus pandemic: the accidental handshake, hugging our friends or cheek kisses as greetings.
You know you shouldn’t, and yet, it...
16 / March / 2020
How the new coronavirus could change our behaviour
We’ve all experienced it during these times of the coronavirus pandemic: the accidental handshake, hugging our friends or cheek kisses as greetings.
You know you shouldn’t, and yet, it...